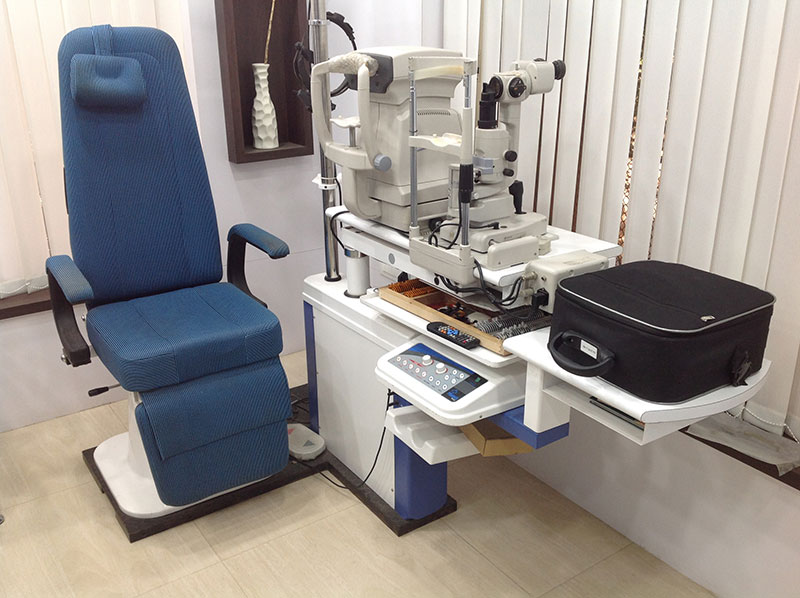
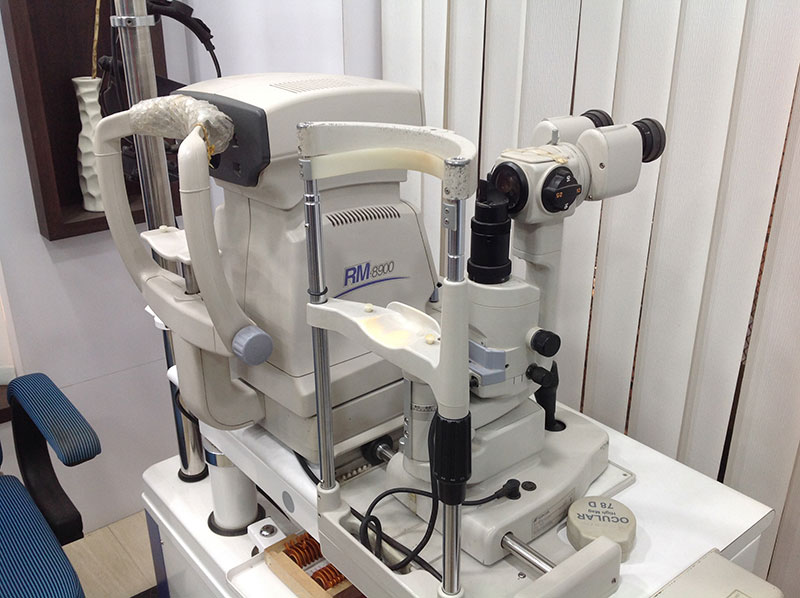
Laser is a highly concentrated light that is beamed onto the retina to treat the desired area. It is a painless Out Patient procedure, lasting about 10-30 minutes that does not require admission. It may require more than one sitting to complete the treatment. In majority of cases, the aim of laser treatment is to try to prevent further loss of vision. It can not regain the vision already lost due to retinal disease. After the laser treatment, the patient may require to undergo repeat Fluorescein Angiography at a later date to monitor the response, and may require more laser if indicated.
Lasers are commonly used in the following conditions:
1. Diabetic Retinopathy
The damaged small vessels of the retina leak fluid and blood, causing swelling of the retina. These changes decrease vision if the central part is affected. Laser is done to seal these leaks. However laser is done to prevent or retard further loss of vision and not to improve vision. In severe changes when new blood vessels have grown (Proliferative Diabetic Retinopathy), multiple sittings of laser are needed to regress these vessels. This is called Pan Retinal Photocoagulation and is highly effective in preventing severe visual loss due to recurrent bleeding in vitreous.
2. Retinal tears and holes
In a retinal tear or a hole without a retinal detachment, laser is done prophylactically to seal the hole and prevent or limit the detachment.

YAG Laser Capsulotomy
1. What is a YAG laser posterior capsulotomy?
It is a non-invasive laser procedure to eliminate the cloudiness that occasionally interferes with a patient’s vision after cataract surgery. During cataract surgery the cataract is removed but a thin membrane that held the cataract is left in place to hold the implanted artificial lens. Leaving the capsule in place during cataract surgery allows the vision after surgery to be more stable and ensures fewer surgical complications. However, sometimes the posterior or back portion of the capsule becomes cloudy over time. This can be resolved with a quick laser procedure performed in the outpatient clinic.
A posterior capsulotomy is for those who have had cataract surgery & whose vision is being affected by cloudiness.
The YAG laser is used to create an opening in the centre for the cloudy capsule. The opening allows clear passage of light rays and eliminates the cloudiness that was interfering with your vision.
2. Realistic expectations
Serious complications with posterior capsulotomy are extremely rare. It is a safe and effective procedure, but like any medical procedure, it does have some risks. The most common being the rise in pressure within the eye. If this occurs then you may be given drops, or a combination of tablets and drops, to reduce the pressure. There is also a slightly higher risk of retinal detachment and also swelling of the macula both of which are rare. if the laser treatment takes place more than 6 months following original cataract surgery.
Going to an eye specialist experienced with the procedure can significantly minimize the risks involved with posterior capsulotomy. If you and your doctor decide that posterior capsulotomy is an option for you, you will be given additional information that will allow you to make an informed decision about whether to proceed. Be sure to have all your questions answered to your satisfaction.
3. Laser treatment for glaucoma
Laser treatment for glaucoma is used in a variety of ways. Laser can be used for angle closure, when it is applied to form a tiny opening in the iris (known as an iridotomy), or laser is used to treat the ciliary body (either externally or internally), or laser can be applied to the drainage angle (selective laser trabeculoplasty) to lower eye pressure.
4. YAG laser iridotomy
Laser iridotomy is performed as a preventative measure against, or as treatment for, narrow angle glaucoma. It is a relatively simple treatment nowadays, with more modern lasers delivering very little energy (eg 20-30mJ) to make a tiny opening in the iris, tucked away under the upper lid. The iridotomy is usually positioned just to one side of the “12 o’clock” position, and in size it is less than 1mm in diameter. The laser treatment typically takes less than 5 minutes, although drops are given beforehand (pilocarpine drops) in most cases so that the laser opening is positioned as peripheral as possible, minimising glare symptoms. Recovery after YAG PI(peripheral iridotomy) is quick, typically 2-3 days. A short course of topical steroid drops after treatment helps to keep the eye comfortable as there can be some sensitivity to light for a few days after treatment.
 5. Selective laser trabeculoplasty
5. Selective laser trabeculoplasty
SLT treatment lowers eye pressure by treating the drainage angle – the trabecular meshwork. It typically lowers IOP (eye pressure) by several points, and lasts for years in most cases. Like all treatments for glaucoma, the effect can wear off in time. This is important to understand, as in many chronic conditions (for example like arthritis) the treatments are aimed to prevent the situation from getting worse (in the case of glaucoma by lowering IOP to a safe level), rather than from curing the condition. Unfortunately, any field lost from glaucoma is invariably permanent, however the good news is that every point of IOP lowering makes the risk of progression of glaucoma lower. SLT also helps to reduce the fluctuations in eye pressure noted more so in glaucoma patients.